
Our Location
Opp. Gulbai Tekra Approach BRTS Stand,
University to Panjrapole Road, Ambavadi,
Ahmedabad, Gujarat 380015
Kidney Transplant
Transplantation offers patients with renal disease the opportunity to be free from dialysis. During a kidney transplant, a new kidney from a living donor (blood related)—or from a patient who has died—is placed within the patient with kidney failure (recipient) by a surgical procedure.
Once patients reach End Stage Renal Disease (ESRD) they will require treatment to perform the function usually performed by the kidney. Two options are available: dialysis and transplantation. Dialysis involves using a machine (hemodialysis) or special fluid placed in the abdomen several times per day (peritoneal dialysis). Along with medication and diet restrictions, these treatments can allow patients to live with renal failure for many years.
Transplant surgery began in the early 1960s. Initially, transplantation was limited to identical twins. Next, new medications allowed transplantation between non-identical relatives, and eventually from related donors, including deceased donors to even ABO incompatible donor now.
Patients were initially treated with very strong medications to prevent rejection of the new kidney. As a result, patients often became ill simply from these medications, and needed to stay in the hospital for a long time.
Since the early days of transplantation, over 100,000 people have received renal (kidney) transplants. Over the last 40 years, a kidney transplant has become a routine procedure. Patients are usually in the hospital for no more than 3-5 days and can return to a very active life. The medications have improved significantly and now have very few side effects for the recipient.
A kidney transplant allows for a regular diet and greater independence than dialysis (removing waste from the blood by a machine). A transplant will likely allow you to return to work. For an appropriate candidate, kidney transplantation is a life-saving procedure. Compared to patients on dialysis, patients receiving a kidney transplant live longer and have a better quality of life.
Kidney transplant is not right for every person on dialysis. People with certain conditions are not eligible for transplantation. These conditions include severe heart disease, active or recent cancer, active infection (including HIV), and the inability to understand and participate in your medical care.
The other main side effect of a kidney transplant is that you will have to take medication every day, exactly as prescribed, for as long as the kidney works. This may mean for the rest of your life. There is a very small increase in some types of infections and cancers—including lymph node and skin cancer—after a kidney transplant.
It is important to remember that this choice is ultimately your decision.
- 95% of the people who have kidney transplants are alive after one year compared with a 90% chance of being alive after the first year of dialysis. For patients with certain conditions—such as diabetes—the risk of death on dialysis is even higher.
- If the kidney comes from a living donor, the success rate is higher than if the kidney came from a deceased person (cadaveric donor). The survival of the transplanted kidney itself is 75% to 85% at one year when it is from a deceased, unrelated donor, as compared to over 90% when the kidney is donated by a living person.
Anyone who has kidney failure can be considered for a transplant, except those with an active infection, cancer, HIV (human immune virus), an autoimmune disorder, obesity, significant heart disease, or severe vascular disease. To become a candidate for transplantation, you must complete a series of medical tests. If you are approved, the transplant team will explore options for donated kidneys. There is often a waiting list for cadaveric kidneys.
Typical patient journey: Kidney transplant
Initial patient evaluation with the transplant team
The team reviews in detail the patient's medical history and current physical condition. The patient will meet the transplant team, including the:
- Transplant surgeon, who examines the patient and discusses the transplant procedure.
- Transplant physician, who reviews the patient's medical history and performs a complete examination to identify conditions which may complicate a future transplant, such as heart disease.
- Transplant coordinator, who tells the patient about the process of getting listed for a donated organ, and about the medications the patient will need after the transplant.
- Dietitian, who discusses dietary restrictions before surgery with the patient, and suggests changes to the diet after successful surgery.
- Social worker, who helps the patient use support resources before and after the transplant.
- Transplant ethical committee examines and evaluates the whole case including both recipients and donors and issues permission for transplantation in accordance with organ transplant act.
Medical tests
In order to determine if the patient is a good candidate for a transplant, the transplant team will ask the patient's primary care physician (family doctor) to order several medical tests. These tests will identify any conditions that might cause problems during the transplant surgery, and help make sure that a transplant is the best treatment option.
Listing for transplant
Based on the evaluation and medical tests, the transplant team will decide if the patient is to be placed on the list for transplantation surgery.
Identifying a donor
There are two sources of donated kidneys: those from living donors and those from patients who have died (cadaveric donors). Kidneys from living donors provide the longest lifespan for both the patient and the kidney. Such kidneys can come from a living relative (brother, sister, parent, etc.), or from a living person not related by blood to the person who will receive the transplant (such as a spouse, adoptive parent ).
Transplant waiting list
If it is not possible to arrange for a living donor, the patient is placed on the waiting list for a cadaveric donated kidney. While waiting for a cadaveric donated organ, a patient must:
- Stay as fit as possible
- Go to all routine health care visits, including dental checkups, flu shots, EKGs, stress testing, colorectal exams, mammograms and pap smears for women, and prostate exams for men.
- Let the transplant center know immediately if the patient has a blood transfusion
- Submit monthly blood samples. If the patient is on hemodialysis, the dialysis center can do this.
- Let the transplant center know of any changes to the patient's address or phone number
- Let the transplant center know of any changes in the patient's health status
Surgery
- Living donor: The date and time of the operation is coordinated with the patient and donor. The patient comes to the hospital on the morning of the operation. The patient is prepared for surgery in the same day surgery center, and will begin taking immunosuppressant medications. The patient is then taken to the operating room for the transplant.
- Cadaveric donor: Patients waiting for a cadaveric donor will be contacted once a kidney becomes available. The transplant coordinator will call, make sure the patient is in good health, and tell the patient what time to arrive at the hospital. Upon arrival, the patient will be examined and will begin taking immunosuppressant medications. The patient is then taken to the operating room for the transplant.
Hospital stay
For a kidney transplant, the patient will be in the hospital for a minimum of three days.
Clinic visits
At discharge from the hospital, the patient will receive an appointment card for a follow-up clinic visit. This is usually for the third day after discharge from the hospital. At this first visit, the transplant team will take some lab tests to track the patient's progress and find any potential problems.
The patient will have regular clinic visits for at least six months. After that time, the patient will return to his or her endocrinologist for regular care.
Kidney transplant surgery
For patients undergoing living donation, the date and time of your operation will be coordinated with you and your donor.
You will come to the hospital on the morning of your operation. We ask that you do not eat anything after midnight and take your medicines with only a sip of water. Next, you will be prepared for your surgery in our same day surgery centre and will begin taking immunosuppression medications. You will then be taken to the operating room for your transplant.
For those patients waiting for a cadaveric donor, you will be contacted once a kidney becomes available. The transplant coordinator will call you, make sure you are in good health, and tell you what time to arrive at the hospital. You should have nothing to eat or drink until your transplant. Upon arrival, you will be examined and will begin taking your immunosuppressant medications.
Regardless of the donor type, the kidney transplant operation is the same. First, the recipient is placed under general anaesthesia. When the patient is safely asleep, the transplant surgeon makes an incision on the right or left side of the lower abdomen, just above the groin.
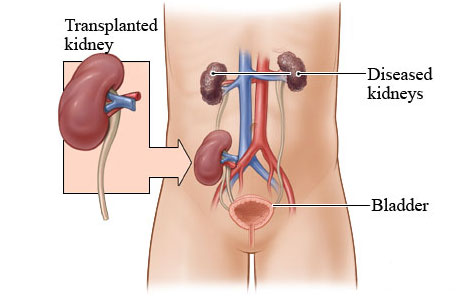
The surgical team will then place the donor kidney into the abdomen and connect the kidney's blood vessels to the recipient's iliac artery and vein, which supply the leg. The surgeons will then connect the ureter (the duct that carries urine) to the bladder. A Foley catheter in the bladder is also used to drain urine and allow the bladder to heal. The surgeon may place a small tube (a stent) within the ureter to insure proper healing. This stent is removed two weeks after surgery by a urologist. In addition, a small drain, called a tube drain is occasionally placed into the abdominal cavity to drain any excess fluid.
You will be in the hospital for a minimum of three days. You may need to stay longer if a problem occurs and further treatment is needed. You can eat on the day after surgery and you will be expected to walk around on the same day. You will be discharged when you can eat and drink, your pain is well controlled with pain pills, and the kidney is functioning well.
After a kidney transplant
Once your transplant surgery is over and the initial anxiety of caring for your new kidney subsides, you should resume as many of your normal activities as possible.
Use the following links to learn more about precautions you need to take after kidney transplant surgery:
- Precautions
In general, you can participate in the activities that you did before your transplant. However, you will need to take some extra precautions. - At home
After surgery, you must routinely do some things at home to check for the first signs of any problem. - Your Medications
The key to the success of your transplant is to take your medications exactly as prescribed. - Clinic visits
At these regular visits, you can meet with any member of your transplant team. The visits usually last about thirty minutes.
Kidney transplantation has become one of the mainstays in management of CRF and the success of such procedure has come a long way in imparting a near normal life to such patients.
